Iliotibial Band Syndrome (ITBS for short) gets a lot of bad publicity. When pain sets in at the back, hip or knee the IT band takes the bullet for the real culprits. Who are the real culprits? More often than not, that would be the muscles that actually attach on to the IT band. Finding the root cause of your pain however will require you to put on your detective cap. Here are NINE considerations to help you start moving in the right direction.
Crack the case on your Iliotibial Band Syndrome

-
Trigger Point Treatment
-
Stretching
-
Vary Postures
-
Weight Loss
-
Pacing
-
Movement Assessment
-
Strengthening
-
Orthotics
-
Rotate Shoes
1. Trigger Point Treatment
As we mentioned in the introduction, the muscles that attach to the IT band are normally the true culprits. We have various muscles that attach to the IT band through fascial lines. If we considered common referral patterns, the gluteals, tensor fascia latae (TFL) and vastus lateralis (quadriceps) are often guilty of referring pain to the IT band. Basically, the trigger points you have in these muscles send pain to the IT band. Using a ball or foam roller can usually do the trick. If that is not working you can see a medical professional that performs trigger point dry needling, massage or a variety of other soft tissue treatment techniques.
2. Stretching
Stretching is one of those “buzz” words that can get people very passionate today. Each clinician that you talk to may have varying opinions about stretching. Different techniques for stretching exist. Without going into too much depth, a time and place exists for both static and active stretching. We also utilize contraction of the muscle being stretched or contraction of a rival muscle on the opposite side of the limb to improve flexibility.
All you need to understand for now is that trigger points cause a shortening of local muscle fibers. Compression to a trigger point helps lengthen these muscle fibers, in turn “releasing” the trigger point. Imagine applying firm pressure to a balloon. It starts to widen or lengthen. This is what we are trying to do when applying pressure to a trigger point. From there we add stretching to help maintain and normalize the new muscle fiber length. (Simons, 2002).
Interested in a FREE IT Band Mobility Program? Click Here
3. Vary Postures
Sustained posture rather than “poor posture” is often the problem. Most of us are deskbound these days. That basically means you are stuck in the same position all day. You are wreaking havoc on your glutes because your sit on them…all day. On top of that your hips are constantly flexed leading to shortness in the muscles at the front of your hip and abdominals. The knee is stuck at 90 degrees so that is the position it becomes used to. You are basically creating short, stiff muscles with plenty of trigger points to go around. You can roll and stretch all day, but expect those problems to return if you don’t get a hold on this.
Standing can also be a problem. We think switching to standing desks will be the cure all. But if you stand in one posture all day you are also going to develop stiffness and trigger points in various muscles. Motion is lotion. Try to change positions frequently. At least every twenty to thirty minutes. Set a time or drink loads of water. More water equals more pee breaks! Your brainpower also dwindles after about thirty minutes so stop beating a dead horse and take a two-minute walk.
4. Weight Loss
Yes, yes you already know. This seems obvious, but is overlooked way too often. Dropping some pounds can be the cure all for a host of different ailments. On top of that, assuming you changed your diet and exercised to accomplish that weight loss you have most likely drastically changed the amount of inflammation surrounding your tissues and joints. Exercise also causes endorphin release. The happy chemical that makes you feel better. It basically acts as a pain killer without all those nasty side effects.
5. Pacing
The majority of medical providers are quick to recommend strengthening to correct any musculoskeletal problems. This is not wrong, however we need to ensure that you are pacing correctly with your exercise. Meaning you aren’t going from 0 to 100 MPH. Many people will begin a new workout regimen with full force. Often leading to set backs, such as IT Band Syndrome. Finding a pre-designed running, biking or fitness routine online can help avoid this. Sometimes the best bet is to bite the bullet and see a skilled fitness or medical professional that can create a tailored plan for you.
6. Movement Assessment [gait, running, biking, lifting]
Before you read this section I want to make something clear. If lack of movement is your problem I would skip right over this portion. Steps 1-4 should be plenty for getting you on the right track if you are more sedentary. Gait and running assessments can be found everywhere these days. Physical therapists, chiropractors, podiatrists, kinesiologists and even shoe stores. Changing the way someone walks or runs can be a slippery slope to go down, for anyone. You want to make sure you put yourself in qualified hands.
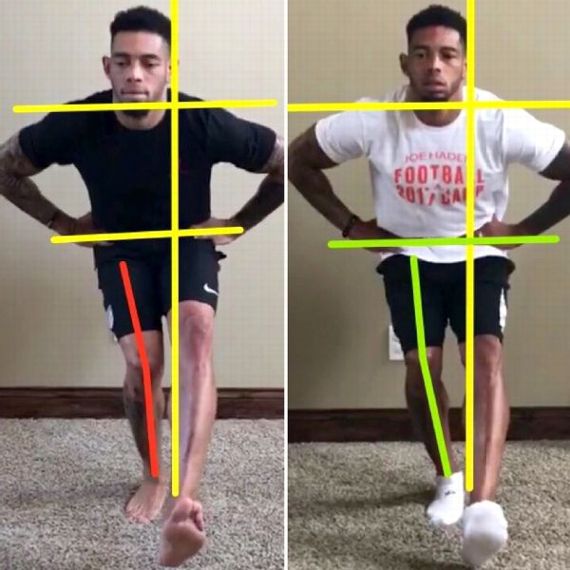
Poor awareness of good alignment at the ankle, knee and hip can often generate some of the pain we see develop around the IT band. Poor alignment when sitting, standing, lifting, walking and running may benefit from corrective exercises. For instance, Joe Haden of the Pittsburgh Steeler’s, has been working on corrective exercises to improve his awareness of alignment at the hip and knee. In an effort to both reduce pain and reduce his risk of injury. In this article, his hip is labeled as “weak” because of the faulty alignment he displays. I would argue that his alignment is more of a compensatory issue than a strength issue. Either way, addressing it may make a difference.
7. Strengthening
I only mention this because many medical providers will convince you that your back, hip or knee pain will return if you do not do four to six weeks of glute strengthening exercises. Lateral knee pain or tenderness around the IT Band does not necessarily mean that you need to spend months rehabilitating. It is possible that the muscles mentioned above are a nagging source of pain because they are not equipped to do what you are asking of them. In this case, re-considering proper pacing strategies in combination with strengthening would be a great idea. If you are sedentary, a general strength program that adds variety will probably do the trick.
Another important consideration is that we see clear strength improvements following treatment of trigger points. Studies have shown that it normalizes muscle timing and strength. On many occasions I will see someone’s hip strength with manual resistance improve dramatically after trigger point dry needling or manual trigger point treatment. Trigger point treatment is not going to turn you into the Hulk, but it may normalize, or “reset,” your current muscle capacity (Lucas, 2004).

8. Orthotics
Excessive pronation, or collapse, at the inside portion of the foot has been correlated with pain around the IT band. Keep in mind that many people display a collapsed arch while walking without IT band pain. These are just general recommendations. As mentioned earlier, receiving a walking or running analysis is a more tailored approach.

9. Rotate Shoes
How long have you had those sneakers you exercise in or those shoes you wear to work? You want to make sure that you are changing your shoes frequently. In the running world somewhere between 300-500 miles is recommended. It clearly depends on how often you are using them. If the shoe no longer sits flat on the ground while it rests on your mudroom floor it is time for a change. Rotating shoes is also a good way to slow down shoe wear. The longer you wear a pair of shoes the more you wear the shoe down in certain locations specific to how you move. This tends to exaggerate any movement faults you have when walking, running, squatting, etc.
Overview
There you have it. Nine ways to help crack the case on your Iliotibial Band Syndrome. The biggest takeaway is that your IT band is not necessarily the problem. It all starts with us. We need to ask ourselves:
- Can we add more variety in our daily postures?
- Can we adjust our workout programming or put more emphasis on our mechanics when running or lifting?
- Could we benefit from dropping a couple of pounds?
From there, we need to address the muscles that are attaching on to the IT band. This should reduce the pain while we work on fixing the true problem. Allowing you to get back to the activities you love to do and the ones you know you need to do.
-Dr. Michael Infantino
Gose, J. Schweizer, P. Ilitobilial band tightness. JOSPT, April 1989.
Lucas KR, Polus BI, Rich PS. Latent myofascial trigger points: their effects on muscle activation and movement efficiency. J Bodyw Mov Ther. 2004;8:160-166
Shamus, J., & Shamus, E. (2015). THE MANAGEMENT OF ILIOTIBIAL BAND SYNDROME WITH A MULTIFACETED APPROACH: A DOUBLE CASE REPORT. International Journal of Sports Physical Therapy, 10(3), 378–390.
Simons, D. Understanding effective treatments of myofascial trigger points. Journal of Bodywork and Movemment Therapies. April 2002.
http://www.espn.com/blog/nflnation/post/_/id/265877/inside-the-physical-re-imagination-of-steelers-corner-joe-haden
https://www.uptodate.com/contents/iliotibial-band-syndrome






